22A06: Exam Report
Describe the cardiovascular changes seen throughout pregnancy
51% of candidates passed this question.
It was expected that candidates would give a detailed description of the changes that occur throughout pregnancy, labour and post-delivery (a timeline).
This should include but not be limited to, cardiac output, total peripheral resistance, blood flow distribution, uterine blood flow and blood volume changes.
Better answers were able to relate these changes to the underlying mechanisms (such as progesterone induced vasodilatation etc). A detailed description of aortocaval compression and its importance was also required. Vague and imprecise statements attracted fewer marks (for example simply stating that heart rate increases without discussing the magnitude, time course and influences).
This topic is well covered in some of the recommend texts.
16A07: Exam Report
Describe the cardiovascular changes of pregnancy including parturition.
62% of candidates passed this question.
Significant CVS changes can occur by eight weeks and then progressively over the term of the pregnancy. Structured answers helped candidates avoid missing important areas of the answer. It was expected candidates could detail the major changes such as a 40 – 50% increase in blood volume, a 30 – 50% increase in cardiac output, a slight decrease in blood pressure, the heart size and position changes, the impact of aortocaval compression and alterations in colloid osmotic pressure. Some mention of the changes during labour and delivery was expected noting uterine contraction squeezes blood to maternal circulation (auto transfusion), cardiac output increases (immediately after delivery up by about 60 – 80%) and blood pressure increases (both systolic and diastolic) during labour.
Hormones, particularly the effects of foetoplacental production or transformation of hormones, and their cardiovascular effects, especially on total body composition / filling pressures were under explained. The cardiovascular changes at parturition were not well explained.
V1i / 22A06 / 16A07: Describe the cardiovascular changes of pregnancy, including partuition
CVS ∆ in pregnancy for:
- Metabolic demands of foetus
- Physiological stress of labour
Timing
Changes commence in early pregnancy, peak 2nd/early 3rd trimester, remain steady until delivery
First Trimester
Maternal systemic VD
Decrease SVR 40%
Second Trimester
Plateau of SVR drop
Steady non- linear increase CO
Third Trimester
CO peaks early 3rd
HR rises 16bpm above non-pregnant values
Supine position reduces CO, SV and increases HR
Pregnancy
↑ CO
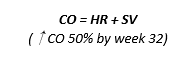
- ↑HR 25%
- ↑SV 30%
- Steady ↑CO from:
- ↑VR → venodilation
- ↑circulating volume → Ostrg activated RAAS
- Large amount of CO going to uteroplacental circulation which is 1L/min at term
- Majority↑CO distributed to placenta, kidneys and skin, providing fetus with nutrients, excretion of waste and maternal temperature control
↑ HR
- Rises steadily from 1st trimester and peaks in 3rd
Contractility
- Improves w pregnancy
- Increase LV mass 40g by 3rd trimester
- PCWP remains normal as hypervolaemia is balanced by ↓PVR
↑ Blood volume
- Blood vol ↑5L 2° Ostrg induced RAAS activation
- ↑Red cell vol 2° ↑EPO
- ↑Plasma vol > red cell vol ∴ ↓HCt ~30%
- Physiological Anaemia of Pregnancy
- ↓Colloid osmotic P → oedema
- Hypervolaemia = ↓Blood viscocity
↓ SBP & ↓ DBP
BP = CO x SVR
- SVR ↓30% below normal values & stays there
- Vasodilation 2° Prgst, prostacyclin, NO, PGIs, downregulation α-receptors
- Necessary to feed placenta → low R circuit
↑ BF to tissues
- Uteroplacental circulation 750mL/min at term
- ↑RBF 80%
- ↑BF breasts, skin, GI tract
↑ O2 delivery
DO2 = CaO2 x CO
- Due to ↑CO
- Compensates for physiological AN
Aortic – Caval Compression
- Compression of IVC & Desc. aorta by gravid uterus
- By 20/40 uterus approaches umbilicus
- IVC compression → ↓VR → ↓CO
- Aorta compression → ↓uterine perfusion, causing:
- Alternative route of VR: epidural Vs → Azygos v.
- ↑ tone → ↑HR, VC → ↑CO
- L) tilt relieves
Partuition
- Uterine contraction → 300mL blood squeezed from uterus back to maternal circulation
- ↑CO% 15 latent phase
- ↑CO 45% expulsive phase
- ↑SBP & DBP ~20mmHg during uterine contraction
Post Delivery
- CO is ↑80 % !!! → due to autotransfusion
- CO & BP returns to normal in 2/52