F10i / 16A02 / 14B03: Describe the Physiological Consequences of PEEP
16A02: Exam Report
Describe the respiratory and cardiovascular effects of applying 10 cm of PEEP (positive end-expiratory pressure) to a healthy mechanically ventilated adult.
29% of candidates passed this question.
This topic has been asked previously. It was expected candidates could detail the impact of PEEP on a variety of respiratory parameters such as lung volume, dead space, arterial pO2 and intrapleural pressure. The cardiovascular consequences are well described including the effect on cardiac output, blood pressure and oxygen delivery.
The physiological impact of lower levels PEEP in a young healthy person is different to that often seen in the critically ill and this was not appreciated by most candidates.
14B03: Exam Report
Describe the physiological consequences of Positive End-Expiratory Pressure (PEEP).
27% of candidates passed this question.
Most answers were quite brief and superficial. They simply did not cover enough of the required knowledge base to gain a pass mark. A definition of PEEP is a useful way to start this answer and this was missing in more than half the answers. Deficiencies in knowledge included even the primary respiratory and cardiovascular effects of PEEP. Many candidates incorrectly concluded
that PEEP would increase afterload and decrease pulmonary vascular resistance. Some candidates provided description of the cardiovascular effects of Valsalva, which was not part of the question. It was expected candidates would also mention physiological effects on other organ systems such as potential cerebral and renal effects.
This topic (Level 1) requires a detailed knowledge and candidates should read widely to gain the depth of understanding required. The core material is covered in texts such as Nunn’s’ Applied Respiratory Physiology and additional applied information can be found in a variety of texts such as Textbook of Critical Care by Fink et al, Irwin and Rippe’s Intensive Care Medicine or Miller’s
Anaesthesia.
F10i / 16A02 / 14B03: Describe the Physiological Consequences of PEEP
Peep Definition
Pressure above atmospheric, maintained at the airways at the end of expiration
Respiratory Consequences
Positive
- ↑Lung Volume
- PEEP = ↑Alveolar P throughout resp. cycle
- Transmural Pressure = PALV – PATM
- PEEP = ↑Alv P
= ↑Transmural P
= Resets FRC according to Lung Compliance
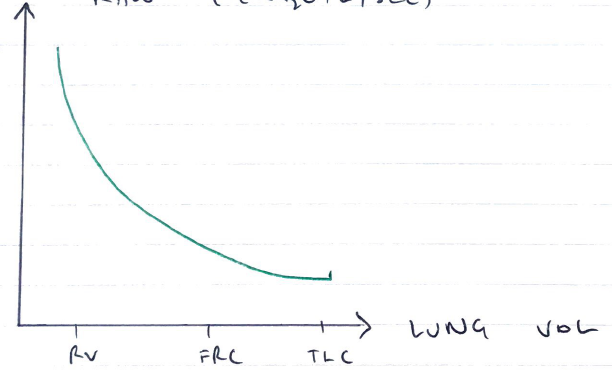
- ↓Airway Resistance
- ↑lung vol = ↓RAW
- RAW (cm H2O/L/sec)
- ↑lung vol = ↓RAW
- ↓V/Q Mismatch
- ↑PALV prevents alveolar collapse at end of expiration
- ↑PaO2
- ↑SA for gas exchange
- Displaces extravascular lung H2O
- ↓WoB
- Overall ↓WoB due to patency of alveoli at end expiration & roll on benefits to resp system
Negative
- Barotrauma
- ↑Transpulmonary pressure gradients >50cm H2O = very high risk rupture of alveolar units, bronchioles & bullae
- ↑PVR
- ↑PALV = ↓diameter intra-alveolar vessels = ↑PVR
- ↑Dead Space
- Long-Term PEEP = bronchiolar dilatation = ↑Dead Space
Cardiovascular Consequences
Negative
- R) Heart
- ↓RV Preload
- 2° ↑intrathoracic P
- ↑RV Afterload
- 2° ↑PVR
- IV Septum Displacement
- 2° ↑RV EDV (from ↑ RV afterload)
- → IV septum bulging → ↓LV filling → ↓CO
- ↓RV Preload
- ↓CO
- ↓CO proportional to ↑Intrathoracic P
- ↑ITP → ↓VR → ↓CO
- ↑ITP → pericardial compression → ↓atrial & ventricular compliance → ↓CO
- Magnified by hypovolaemia
- ↓O2 Flux
- DO2 = CO x CaO2
- PEEP = ↑PaO2 ∴↑CaO2 but ↓CO much greater → ↓DO2
Renal Effects
- ↓Renal perfusion
- ↓GFR
- ↓UO
- ↑ADH, ↑ANP
↓CPP
CPP = MAP – (CVP / ICP)
- PEEP → ↓MAP & ↑CVP / ICP → ↓CPP
- ↑intrathoracic P → ↑CSF pressure & intracranial P
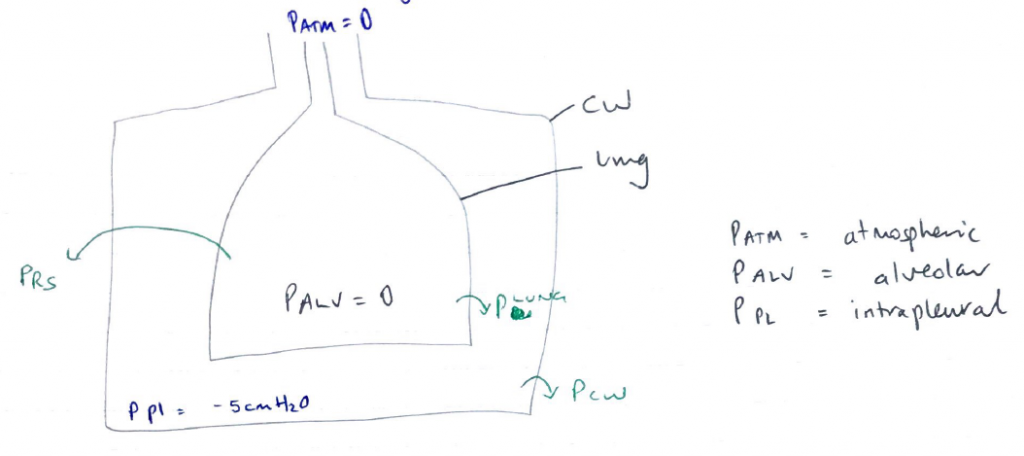
Notes on Transmural Pressure
- Pressure inside relative to outside of a compartment
- Transmural P lungs KA TRANSPULMONARY P
- P Resp System = PALV – PATM
- PCW = PINTRAPLEURAL – PATMOSPHERE
- PLUNG = PALVEOLAR – PINTRAPLEURAL
- Lungs have tendency to recoil inwards
- Inflating lungs requires ↑transpulmonary P (to create difference between alveoli & atmosphere)
- You can ↑transpulmonary P (P Resp system) by:
- ↑PALVEOLI
- ↓ outside P (ATM)
- Author: Krisoula Zahariou