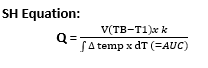G6iii / 17B10: Compare and contrast two methods of measuring cardiac output
17B10: Exam Report
Compare and contrast two methods of measuring cardiac output.
35% of candidates passed this question.
Good answers began with a definition of cardiac output. For each method, it was expected that candidates discuss the theoretical basis, equipment, advantages and disadvantages / sources of error and limitations. Additional marks were awarded when an attempt was made to compare and contrast the two methods (often helped by the use of a table).
G6iii / 17B10: Compare and contrast two methods of measuring cardiac output
Cardiac Output
- CO = HR x SV = volume of blood ejected by heart per minute
- Determinants of CO are HR and SV
Techniques to Measure CO
Inavasive
Non Invasive
PAC
- Dye Thermodilution
Fick Principle
TTE
TOE
Oesophageal Doppler
Pulse Contour Cardiac Output
- PICCO
- LiDCO
Partial CO2 rebreathing
Dye Thermodilution
Transoesophageal Echocardiography
Theory
CO measurement is based on the FICK PRINCIPLE
“Amount of indicator substance taken up over time = A – V difference of the substance x blood flow”
- Current thermodilution practice of measuring CO uses a modified STEWART HAMILTON EQUATION
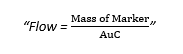
- The marker is temperature
Uses Doppler technique to monitor cardiac function by multiplying the velocity-time integral (VTI) of blood flow through the transversal area of the vessel (CSA) with HR
CO = CSA * VTI * HR
Equipment
Thermistor-tipped Swan Ganz Catheter
Cold D5W
STEPS
- Bolus of sterile solution (injectate) colder than pt blood is injected into RA port
- Injectate mixes with RA blood → TV → RV → PA
- Thermistor located 4cm from tip of catheter situated in PA detects ∆blood temp as blood passes catheter tip
- Temp ∆ detected produces a curve which shows: ∆TEMP vs TIME calculated by a computer & converted into a measurement of CO by S – H application
Q = CO
V = volume of injectate
TB = temp blood
T1 = temp injectate
K = constant, which corrects for specific heat & density of inectate
dt = ∆ time
- AuC is inversely related to CO
- Small AuC = quick CO
- Larger AuC = slow CO
- Mean of 3 measurements is taken
- Mean has to be 15% different to previous mean → otherwise there has been a margin of error
- Transoesophageal ultrasound transducer
- Skilled operator
- Anaesthetised patient
The TOE probe is introduced into the mouth and passed down the oesophagus to visualise the Aortic Valve then
inserted to the gastric cavity to obtain transgastric view of LVOT
Aortic Blood flow is obtained by pulsate Doppler
The VTIAORTIC os calculated by outlining the Aortic blood flow
Advantages
- Non-toxic indicator
- Repeated measurements easily
- Computer performs all patented algorithms
- Direct measurements in real time
- Cardiac anatomy
Disadvantages
Associated w increased M&M:
- Arterial injury
- PTx
- Chylothorax
- Nerve injury
- PA rupture
- Valve damage
- Risk of oesophageal perforation
- Odynopahgia
- Harmorrage
- ETT malpositioning
- Dental injury
Error/Limitation
Factors compromising technique:
- Shunts
- TR
- Cardiac Arrythmias
- Abnormal respiratory patterns
- Low CO state
Assumes:
- Constant flow
- Normal heart & valves
- No resp. fluctuations
- Requires advanced training & expertise
Comparison
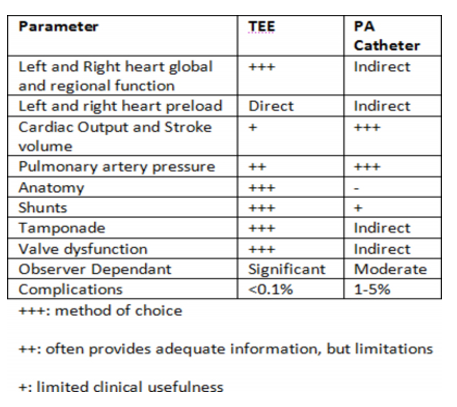
- PAC: constant PAP, frequent CO, sampling of SVO2 – however these values are modified by artificial ventilation and ventricular non compliance
- TOE: gives direct measurements of values whereas PAC is indirect. Most PAC values can be calculated by TOE, except for SVO2
- Safety: PAC has a higher complication rate (1-5% cf TOE 0.1-0.2%)
- Author: Krisoula Zahariou